Regenerative Medicine in Pain Management
Regenerative medicine has emerged as a promising frontier in the management of acute and chronic pain, shifting the paradigm from symptomatic relief to tissue repair and restoration of function. Traditional pain management strategies—such as pharmacological therapy, nerve blocks, and surgery—often focus on alleviating symptoms rather than addressing the underlying pathology. In contrast, regenerative approaches aim to harness the body’s intrinsic healing mechanisms to repair damaged tissues, thereby offering the potential for long-term relief and improved quality of life.
At its core, regenerative medicine involves the use of biological therapies such as platelet-rich plasma (PRP), stem cells, growth factors, and tissue engineering techniques. These therapies are designed to stimulate healing, reduce inflammation, and promote regeneration of musculoskeletal structures including cartilage, tendons, ligaments, and intervertebral discs—common sources of chronic pain.
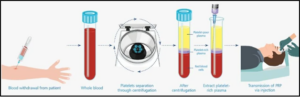
Platelet-Rich Plasma (PRP) is one of the most widely used regenerative therapies in pain management. PRP is derived from the patient’s own blood, which is centrifuged to concentrate platelets rich in growth factors. When injected into injured tissues, PRP enhances cellular repair, angiogenesis, and collagen synthesis. It has been used effectively in conditions such as osteoarthritis, tendinopathies (e.g., tennis elbow, Achilles tendinitis), and ligament injuries. Clinical studies have shown that PRP can reduce pain and improve function, particularly in early stages of degenerative diseases.
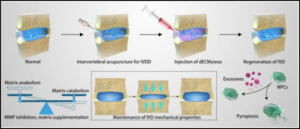
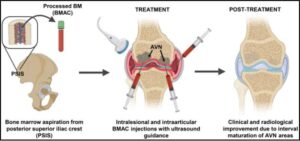
Stem cell therapy represents another key modality in regenerative medicine. Mesenchymal stem cells (MSCs), typically harvested from bone marrow or adipose tissue, have the ability to differentiate into various cell types such as cartilage, bone, and muscle. In addition to their regenerative capacity, MSCs exert anti-inflammatory and immunomodulatory effects. In pain management, stem cell therapy has shown promise in treating osteoarthritis, degenerative disc disease, and chronic joint pain. Although still under investigation, early results suggest that stem cell therapy may slow disease progression and provide sustained pain relief.
Growth factor therapy and biologics further enhance the regenerative process. Growth factors such as transforming growth factor-beta (TGF-β), platelet-derived growth factor (PDGF), and vascular endothelial growth factor (VEGF) play crucial roles in tissue repair. These molecules can be delivered directly or released from PRP and stem cells to accelerate healing. Advances in biotechnology have also enabled the development of engineered scaffolds that support tissue regeneration by providing a structural framework for cell growth.
Regenerative medicine has relevance in the management of chronic musculoskeletal pain, where conventional treatments often fall short. Conditions such as osteoarthritis, chronic low back pain, and sports injuries are associated with tissue degeneration and inflammation. By targeting the underlying pathology, regenerative therapies offer a disease-modifying approach rather than temporary analgesia. This is especially important in the context of the global opioid crisis, as regenerative medicine provides an alternative to long-term opioid use and its associated risks.

Regulatory and ethical considerations also play a significant role. The use of stem cells, in particular, is subject to strict regulations to ensure patient safety and prevent misuse. Furthermore, the cost of regenerative therapies can be high, limiting accessibility for many patients. Insurance coverage remains inconsistent, which may hinder widespread adoption.
Another important aspect is patient selection. Not all patients are ideal candidates for regenerative therapies, and outcomes may vary depending on factors such as age, severity of disease, and overall health status. Therefore, careful evaluation and individualized treatment planning are essential to achieve optimal results.
Looking ahead, the future of regenerative medicine in pain management is highly promising. Advances in molecular biology, gene therapy, and tissue engineering are expected to enhance the effectiveness of these therapies. Personalized medicine approaches, where treatments are tailored to the patient’s genetic and biological profile, may further improve outcomes. Additionally, combining regenerative therapies with rehabilitation and physical therapy may yield synergistic benefits.
In conclusion, regenerative medicine represents a transformative approach to pain management by focusing on healing rather than merely alleviating symptoms. While challenges remain, ongoing research and technological advancements are likely to expand its role in clinical practice. As evidence continues to evolve, regenerative therapies may become a cornerstone in the management of chronic pain, offering patients safer and more sustainable relief.



